
Scarlet fever is an acute infection with a primary lesion of the oropharynx, severe poisoning and characteristic rash. The cause of scarlet fever is group A streptococcus, which is transmitted by the patient through contact or in the air. Scarlet fever clinic includes general poisoning and fever, scarlet fever, regional lymphadenitis, raspberry tongue, petechial rash, followed by pepper on the skin. The diagnosis of scarlet fever is based on the appearance of typical clinical symptoms.
Scarlet fever
Scarlet fever is an acute infection with a primary lesion of the oropharynx, severe poisoning and characteristic rash.
Characteristics of the pathogen
Scarlet fever causes beta-hemolytic streptococcal group A, Gram-positive, optionally aerobic, ovoid form of Streptococcus bacteria. The reservoir and source of the scarlet fever, as with all streptococcal infections, is a man: sick or sluggish. Patients with scarlet fever are the most dangerous in the first days of the disease. The likelihood of transmission of the infection completely disappears three weeks after the onset of clinical symptoms. Significant percentage of the population (15-20%) relates to asymptomatic infection carriers, sometimes people have been months and years the source of infection.
Streptococcus is transmitted through an aerosol mechanism (the patient releases the pathogen when coughing, sneezing, while talking) air or contact. If the pathogen is in contact with food, the implementation of the food routine is possible. The infection is most likely due to close contact with a sick person.
The natural susceptibility of humans to scarlet fever is quite high, the disease develops in individuals infected with beta-hemolytic streptococci (erythrogenic toxin release) in the absence of antitoxic immunity. The immunity formed after infection is type-specific and does not prevent infection by another type of streptococcus. There is a seasonal dependency: the incidence increases in the autumn-winter period; as well as communication with other respiratory streptococcal infections (sore throat, streptococcal pneumonia).
Pathogenesis of scarlet fever
The gateway to the scarlet fever is the pharynx mucosa, nasopharynx, sometimes (extremely rare) genitals. It happens that bacteria get into the body through skin damage. A local focus of infection with characteristic necrotic phenomena forms in the area of the introduction of the pathogen. When breeding breaks out, microorganisms release toxins into the blood, contributing to the development of infectious poisoning. The presence of toxin in the general bloodstream stimulates the expansion of small vessels in various organs, especially skin integument, which manifests itself as a specific rash.
Anti-toxic immunity is gradually formed, which helps to reduce the signs of intoxication and the disappearance of rash. Occasionally, direct pathogens enter the blood, causing other organs and tissues to be defeated by microorganisms (lymph nodes, meninges, temporal bone tissue, hearing aids, etc.), causing purulent necrotic inflammation.
Scarlet fever symptoms
The incubation period can last from days to ten days. The disease begins acute, the temperature rises sharply, accompanied by signs of increasing poisoning: headache, muscle pain, weakness, tachycardia. A high fever on the first day is often accompanied by increased mobility, euphoria, or vice versa: apathy, sleepiness and lethargy. Significant toxicity can cause vomiting. Recently the course of scarlet fever with moderate hyperthermia has been observed, not reaching high numbers.
Pain in the throat when swallowing. Examination of the pharynx shows pronounced hyperaemia of the tonsils (much more intense than with angina), tongue arms, behind the neck, soft palate (the so-called "flaming snap"). At the same time, the hyperemia of the mucous membrane is clearly limited by the point at which the soft palate changes to hard. Sometimes the clinical picture of follicular-lacunar tonsillitis develops: intensely hyperemic mucosa of the tonsils covered with foci (often small, but sometimes large and deep), raid, mucopurulent, fibrinous or necrotic.
At the same time, regional inflammation (anterior) lymph nodes develops: they increase slightly, feel tight and become painful. Speech, originally covered with greyish-white flowers, subsequently (4-5 days of illness) acquires a rich alo-purple color, papillary hypertrophy occurs. Lips painted with a heavy gait in the same color. General, At this point the angina begins to lower. Necrotic attacks fall back noticeably more slowly.
A characteristic puncture rash occurs on the first or second day of the disease. Against the background of general hyperemia, darker spots appear on the skin of the face and upper body (and later on the flexion surfaces of the arms, sides, inner thighs), condensation on skin folds and in places of natural folds (elbow loop, groin, armpit) and form dark red stripes (symptom pastia).
In some cases, point elements of the rash are merged into a large erythema. For a rash on the face, a localization on the cheeks, temple, forehead. There are no rashes in the nasolabial triangle, here the blanching of the skin is noticed (symptom Filatov). Rash temporarily disappear when pressed on it. Due to the fragility of blood vessels, on the skin, in places, exposed to friction or pressure, minor bleeding may occur. Sometimes small papules, maculae and vesicles are noticed in addition to the scarlet rash. In addition, there is a late rash (for 3-4 days of illness) or lack thereof.
Generally, 3-5 days after the onset of the disease, the patient’s condition improves, and the symptoms gradually decrease, the rash fades and, at the end of the first – the beginning of the second week, completely disappears, leaving small flakes on the Skin (on the palms and feet – large scale). The severity of the rash and the speed of its disappearance vary depending on the severity of the disease. The intensity of the peeling depends directly on the frequency and duration of the rash.
Then an extra-buccal form of scarlet fever occurs when the pathogen is introduced through damaged skin (in places of abrasions, injuries, surgical wounds). At the same time, a purulent-necrotic focus forms in the area of the damage, rashes from the site of insertion and lesions in the throat are not observed.
Deleted form of scarlet fever is sometimes observed in adults, characterized by minor poisoning, moderate pharyngeal catarrh, and scanty, pale, short-term rash. In rare cases (even in adults) scarlet fever is extremely difficult with the likelihood of toxic and septic shock: fulminant progression of the poisoning, severe fever, development of cardiovascular failure. Hemorrhages often appear on the skin. This form of scarlet fever is fraught with dangerous complications.
Scarlet complications
The most common purulent-inflammatory complications in scarlet fever (lymphadenitis, otitis) and late complications, associated with infectious allergic mechanisms (cardites, arthritis, nephritis autoimmune genesis).
Diagnosis of scarlet fever
The high specificity of the clinical picture enables you to make a reliable diagnosis during the questioning and physical examination. Laboratory diagnostics: complete blood count – detects signs of a bacterial infection: neutrophilic leukocytosis, leukocytes shift to the left, increased ESR. RCA is a specific rapid diagnosis. The pathogen is not isolated due to irrationality.
When developing complications of the cardiovascular system, the patient needs a consultation with a cardiologist, EKG and ultrasound of the heart. If otitis occurs, an otolaryngologist and otoscopy are required. To assess the condition of the urinary system, an ultrasound of the kidneys is performed.
scarlet treatment
Scarlet fever treatment is usually done at home, patients with severe forms must be hospitalized. Patients prescribed bed rest for 7-10 days, recommend an economical diet (semi-liquid food) for the period of pronounced anginal symptoms, not to mention the balanced vitamin composition of the diet.
penicillin is this Means of choice for the etiotropic treatment of scarlet fever, which course is prescribed for 10 days. First generation macrolides and cephalosporins are used as reserve medications (in particular: erythromycin and cefazolin). If there are contraindications to the use of the above preparations, synthetic penicillins or linkosamides can be prescribed. The combination therapy of the antibiotic with antitoxic serum is successfully used in complex therapy.
To rehabilitate the source of infection, gargle with a solution of Furatsilina in dilution 1: 5000, infusions of medicinal herbs (daisies, eucalyptus, calendula). In the event of severe intoxication, an infusion of glucose solutions or salts occurs, cardiac anomalies are corrected by suitable cardiology medications (nicetamide, ephedrine, camphor).
Scarlet forecast
Modern medicine can successfully suppress streptococcal infections, including scarlet fever, due to the use of antibiotics in the early stages of the disease. In most cases, the disease has a favorable prognosis. Rare cases of serious illnesses with the development of a toxic septic form of the disease can cause complications. Currently, a disease, generally, is beneficial, but occasionally toxic or septic scarlet fever can occur, usually hard. Recurrent disease occurs in 2-3% cases.
Prevention of scarlet fever
General measures to prevent scarlet fever include timely identification of patients and infectious agents, their proper isolation (at home or in the hospital), implementation of quarantine activities (especially if scarlet fever is detected in kindergartens, schools, medical facilities). Patients are discharged from the hospitals at the earliest on the 10th day after the onset of the disease, after which they are at home for a further 12 days. Patients cannot return to the team earlier than 22 days after a bacteriological test for the presence of the pathogen.
Children who have not previously had scarlet fever and are in contact with patients, no kindergarten or school for 7 days after contact, adult contact persons are observed for 7 days, but without any restrictions at work.
RELATED ITEMS
-

Scarlet fever: causes, symptoms, diagnosis, course therapy
Sudden fever, red cheeks and tonsillitis: these symptoms indicate the infectious disease scarlet fever. A little later show up…
-
Teething – causes, symptoms & treatment
There’s something wrong with Klein-Oliver. He cries lightly, he whines and leaves his favorite toy in the closet unnoticed. Has the child got it?…
-

Scarlet fever in children – tips for prevention – treatment, I am a mother
Health is an issue that parents always have in mind. That is why it is important to be aware of the most common teething problems in order to avoid them…
-
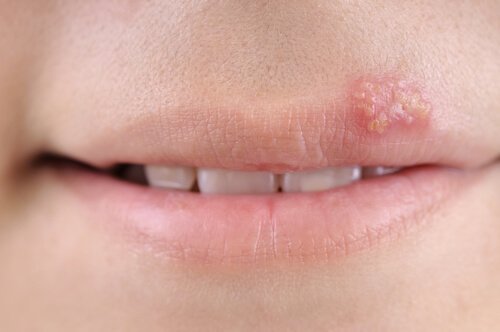
Herpes in children: symptoms, causes and treatment – I am a mother
Because of the high risk of infection, the herpes virus is much more widespread in children than one might think. And once you look at that…
